by J. Clifford* (8/17)
Quick Facts…
- The three cornerstones of diabetes management include a healthful eating pattern, physical activity, and medication, if necessary.
- It is recommended that people with diabetes work with their diabetes management team to develop a nutrition care plan that fits their metabolism, nutrition, and lifestyle needs.
- The overall goals of nutrition therapy include achievement and maintenance of near normal blood glucose and blood pressure levels, optimal blood lipid levels, reasonable weight, the prevention of acute and long-term complications, and optimal nutrition and physical activity.
- The Plate Method is the recommended diet plan for people with diabetes. Other methods include diabetic exchange diets and carbohydrate counting.
Diabetes is a chronic disease in which food is not properly absorbed in the body to be used as energy. This results in high levels of sugar in the blood. During the normal process of digestion, food is consumed and broken down into small sugar particles called glucose. The glucose enters the blood stream and is moved into the body’s cells, where it can be used as energy. Insulin is a hormone that is produced by the pancreas that helps the body store and use glucose. People with diabetes either have too little insulin production, their body is unable to use insulin properly (insulin resistance), or both. This prevents glucose from moving into the body’s cells, which results in high levels of glucose in the bloodstream. There are four major conditions associated with high blood glucose levels: pre-diabetes, type 1 diabetes, type 2 diabetes, and gestational diabetes.
Diabetes encompasses a variety of metabolic complications. It is recommended that people with diabetes work with their diabetes management team (registered dietitian, nurse, physician, and other health care professionals, as needed) to develop a nutrition care plan that fits their own metabolism, nutrition, and lifestyle requirements. The plan should also take into consideration the presence of complications or other medical conditions and include ongoing diabetes
support as an integral component of care. The three cornerstones of diabetes management are: a healthful eating pattern, physical activity, and medication, if necessary (i.e., insulin or oral glucose-lowering agents).
Pre-Diabetes
Pre-diabetes is a term used for people who are at increased risk for developing diabetes. People with prediabetes have blood glucose levels that are higher than normal but not high enough to be diagnosed with diabetes. This condition puts you at a higher risk for developing type 2 diabetes and cardiovascular disease. There are no clear symptoms of prediabetes, but some individuals may have symptoms or problems of diabetes already. There are three tests that may be done by a
doctor to determine if an individual has pre-diabetes. These include the A1C test, the fasting plasma glucose test, and the oral glucose tolerance test. If a person is diagnosed with pre-diabetes, they can still make lifestyle changes to prevent the diagnosis of type 2 diabetes, and to return blood glucose levels to the normal range. Ways to prevent diabetes include keeping a healthy weight (or losing weight if overweight), staying active most days of the week, and eating
lowfat meals that contain many fruits, vegetables and whole grain foods. Research shows that you can lower your risk for type 2 diabetes by 58% by losing 7% of your body weight, and exercising moderately for at least 30 minutes a day for 5 days a week. Even losing 10-15 pounds can make a huge difference.
Type 1 Diabetes
Diabetes is categorized as type 1 or type 2, based on the underlying physiological problem. Type 1 diabetes, formerly known as insulin-dependent diabetes mellitus (IDDM) or juvenile diabetes, is characterized by the destruction of the pancreatic beta cells that produce insulin, causing an insulin deficiency. Only 5% of those with diabetes have this form of the disease. Type 1 diabetes occurs most often in children and young adults, but can occur at any age. With the help of insulin therapy and other treatments, type 1 diabetes can be easily managed.
Type 1 diabetes management includes insulin injections through insulin pens or syringes or an insulin pump, as well as exercise, nutrition, and support. Through daily insulin injections, one can monitor blood glucose levels and administer insulin accordingly. This approach allows a person to adjust the timing and quantity of insulin injected according to their monitored blood glucose levels. Exercise is also a key component to proper diabetes care by contributing to more stable blood glucose levels.
A primary treatment goal in type 1 diabetes should be tight blood glucose control. Frequent blood glucose monitoring is recommended. Blood glucose monitoring can show which foods, physical activities, and times of the day elevate an individual’s blood glucose level. By adjusting insulin dose to meet needs, a person may have more near-normal blood glucose levels, which may help reduce the risk for short- and long-term complications.
Type 2 Diabetes
Type 2 diabetes, previously known as adult-onset diabetes is the most common form of diabetes. In this case, your body does not use insulin properly, this is called insulin resistance. When the problem initially arises, your pancreas will make extra insulin to compensate, but over time it can’t make enough insulin to stabilize blood glucose levels.
Initially, diabetes will cause glucose to build up in the blood stream rather than being transported into cells, which may starve your cells for energy. If uncontrolled, type 2 diabetes can lead to serious long term complications. Complications include heart disease and stroke, blindness and eye problems, kidney disease, nervous system disease, amputations, skin conditions, hearing impairment, and Alzheimer’s disease.
Achieving and maintaining weight loss has long been a primary dietary focus for people with type 2 diabetes. Total calories consumed should be sufficient to maintain a desirable weight and prevent weight gain. Physical activity on a regular basis is recommended. Aiming for blood glucose control, along with normal blood lipid levels and normal blood pressure are also important goals. These factors, if controlled, help reduce the risk of long-term complications of diabetes.
Symptoms of type 2 diabetes develop slowly, but those at risks should be aware of the signs. Some symptoms include increased thirst and frequent urination due to blood sugar buildup, increased hunger due to energy deprivation in cells, weight loss from the inability to metabolize glucose, fatigue, blurred vision, slow-healing or frequent infections, and areas of darkened skin. Although the development of type 2 diabetes is not fully understood, there are some clear factors that increase risk, including: being overweight, fat distribution in the abdomen, inactivity, family history, black, Hispanic, American-Indians and Asian-American races, age over 45, prediabetes, gestational diabetes, and polycystic ovarian syndrome.
Blood glucose testing is essential for controlling diabetes, and keeping a log of your results is recommended. Review your results to understand how food, activity, and stress affect your blood glucose. Note if your levels have been too high or too low around the same time of day, and work with your doctor to understand the details of your results. This process takes time, and may require many revisions to nail down a daily routine.
Gestational Diabetes
Gestational diabetes begins or is first diagnosed during pregnancy. Often times, this type of diabetes may be caused by pregnancy hormones, occurs towards the end of a women’s pregnancy, and will go away once the baby is born. During pregnancy, the placenta produces high levels of various hormones which may impair the action of insulin in cells, raising blood sugar. As the baby grows, more insulin-blocking hormones are produced, and can provoke a rise in blood sugar. Risk factors for gestational diabetes include age older than 25, family history of diabetes, high blood pressure, overweight before pregnancy, unhealthy cholesterol, smoking, inactivity, and unhealthy eating. Women with gestational diabetes during pregnancy are more likely to develop diabetes in the future. Therefore, it is important for women with gestational diabetes to take steps to reduce their risk for developing type 2 diabetes later in life. Eating well during pregnancy is important for all women, regardless of the risk for gestational diabetes.
Diagnosis of Diabetes
Diagnosis of diabetes is determined through A1C levels, fasting plasma glucose levels, oral glucose tolerance tests, or random plasma glucose tests. Criteria for diagnosis of diabetes are:
| Result | A1C | |||
| Normal | Less than 5.7% | |||
| Prediabetes | 5.7% to 6.4% | |||
| Diabetes | 6.5% or higher | |||
| Result | FPG | |||
| Normal | Less than 100 mg/dl | |||
| Prediabetes | 100 mg/dl to 125 mg/dl | |||
| Diabetes | 126 mg/dl or higher | |||
| Result | OGTT | |||
| Normal | Less than 140 mg/dl | |||
| Prediabetes | 140 mg/dl to 199 mg/dl | |||
| Diabetes | 200 mg/dl or higher | |||
Hemoglobin AIC
Hemoglobin A1C is a test that measures the average plasma glucose concentrations over a 2-3 month period of time.
Fasting Plasma Glucose
Fasting plasma glucose is measured when a person has had no caloric intake for greater than 8 hours. The test is usually done first thing in the morning before breakfast.
Oral Glucose Tolerance Test
During an oral glucose tolerance test, a person fasts overnight, and then a fasting blood sample is measured. The individual then consumes a sugary liquid, and blood sugar levels are measured periodically for the next two hours.
Random plasma glucose levels greater than or equal to 200 mg/dL are also a diagnosis for diabetes.
Target Goals
People with diabetes should aim for People with diabetes should aim for goals to lower blood pressure and normalize blood lipid levels. Appropriate target goals for people with diabetes are blood pressure levels are less than 140/90 for most individuals, and a lower target of 130/80 mmHg is appropriate for some if it can be safely achieved. LDL cholesterol less than 100 mg/dL, HDL cholesterol greater than 40 mg/dL for men, and greater than 50mg/dL for women, and triglyceride levels less than 150 mg/dL.
Dietary Recommendations
An initial dietary strategy for those witAn initial dietary strategy for those with diabetes is to improve food choices to better meet the recommendations of the 2015-2020 Dietary Guidelines for Americans and MyPlate released by the U.S. Department of Agriculture. Limiting calories from added sugars, saturated fats, trans fats, and sodium, and increasing physical activity to at least 150 minutes per week are highly recommended. Individuals should plan to eat meals throughout the day to spread nutrient intake. Even mild to moderate weight loss (5-10% of body weight) has been shown to improve diabetes control. Lifestyle changes that moderately decrease calorie intake (250 to 500 kcal/day) and increase energy expenditure are strongly encouraged. Blood glucose monitoring may also be used to determine if lifestyle modifications are sufficient to achieve blood glucose control or if additional medications are necessary to be combined with nutrition therapy.
Protein
A protein intake of .8g/ kg of body weight is recommended for the general population, as well as for those with diabetes. Adult men need about 56 grams per day, and adult women need about 46 grams per day. There is no evidence to indicate the usual protein intake should be modified if kidney (renal) function is normal. A protein intake above 35% of total daily calories may have a detrimental effect in the development of nephropathy (renal disease). The best choices for protein are plant-based proteins, such as nuts, seeds, and legumes as well as fish and seafood, chicken and poultry, cheese, and eggs. Try to include fish in your meal plan at least twice a week. Many plant-based protein foods like beans, soy, and breaded meats will contain carbohydrates, so read food labels carefully.
Fat
The most life-threatening consequences of diabetes are cardiovascular disease (CVD) and stroke, which occur in people with diabetes more often than others. Diabetes itself is a strong independent risk factor for CVD. Thus, steps that help reduce this risk are important, such as choosing heart healthy fats. A person with diabetes should limit foods containing saturated fats, and consume foods containing polyunsaturated fats and monounsaturated fats more often.
Saturated Fat and Trans Fat
Saturated fats are found in high-fat meats, high-fat dairy products, lard, butter, cream sauces, and coconut, palm, and palm kernel oil. They are usually solid at room temperatures and raise LDL cholesterol levels. Individuals with or without diabetes should eat less than 10% of calories from saturated fat. Trans fats are produced when liquid oil is made into a solid form through a process called hydrogenation. The effect of trans fat is similar to saturated fat in raising LDL cholesterol. In addition, trans fat lowers HDL cholesterol, which is not desirable. Foods containing trans fats include stick margarine, shortening, and many processed baked goods like crackers, cookies, and sweet breads. Trans fats are listed on food labels, but to avoid as much trans fat as possible, look for words like hydrogenated oil or partially hydrogenated oil. Select foods that do not contain these ingredients.
Polyunsaturated Fat
Polyunsaturated fats are heart healthy fats, and when eaten in moderation, they may lower cholesterol levels. Polyunsaturated fats are found in fatty fish such as salmon, mackerel, herring, and trout, vegetable oils such as safflower oil and soybean oil, walnuts and flax seeds. Two or more servings of fish per week are recommended for people with diabetes (excluding commercially fried fish).
Monounsaturated Fat
Monounsaturated fats are also heart healthy fats and help to lower LDL cholesterol. Foods high in monounsaturated fats include olive oil, canola oil, walnut oil, peanut oil, avocados, olives, nuts, and seeds.
Omega-3 Fatty Acids
Omega-3 fatty acids are a type of polyunsaturated fat that may be especially beneficial for heart health. Research suggests that consuming omega-3 fatty acids found in fish and fish oils can decrease the risk of coronary artery disease, and may decrease insulin resistance in people with diabetes. There are three types of omega-3 fatty acids. Alpha-linolenic acid (ALA) is found in vegetable sources, eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) are found in fish and other marine life. The richest dietary source of omega-3 fatty acids is oily cold-water fish such as salmon, tuna, trout, sardines, mackerel, and herring. Omega-3 fatty acids can also be found in nuts (especially walnuts), flax seeds, canola oil, tofu and other soybean products, and specially fortified eggs.
Total fat intake for people with diabetes should be 25 to 35% of total calories. Saturated fat should be limited to less than 10% of total calories, and most fat intake should be coming from sources of polyunsaturated and monounsaturated fatty acids. Elevated levels of triglycerides (greater than 150 mg/dl) are also a risk factor for CVD. The addition of exercise may result in greater decreases in total and LDL cholesterol and triglycerides, and prevent a decrease in high density lipoprotein (HDL) cholesterol.
Carbohydrates
Carbohydrates are an important fuel source for the body. They are found in breads, starches, fruit, and dairy. When a carbohydrate containing food is consumed, the carbohydrate is broken down into glucose. Glucose provides fuel for the body and is essential for life. Glucose is carried through the blood stream into the cells with the help of insulin. Once in the cells, the glucose can be used for energy. Carbohydrates raise blood glucose levels, therefore people with diabetes may need to balance carbohydrate intake with insulin, medications, and physical activity. The three main types of carbohydrate found in food are sugars, starches, and fiber.
Sugar
The two main types of sugar include naturally occurring sugars, such as those in fruit and milk, and added sugars, such as those which are added during processing. Current guidelines allow the use of sugar and sugar-containing foods in modest amounts as part of a balanced diet. It should be remembered, however, that sugar-containing foods must be substituted for other carbohydrate foods and not simply added on top of what is eaten. The first dietary consideration for a person with diabetes should be the total amount of carbohydrate eaten. This does not mean that sweets should be eaten with every meal or even every day. Sweets also can be high in calories. Moderation is the key.
Non-nutritive Sweeteners
Many non-nutritive sweeteners have been approved by the Food and Drug Administration (FDA) and can be used by people with diabetes, including pregnant women, within a balanced diet. Because saccharin can cross the placenta, other sweeteners are better choices during pregnancy. The use of non-nutritive sweeteners has the potential to reduce overall calorie and carbohydrate intake if used as a replacement for caloric sweeteners.
Starch
Foods high in starch include starchy vegetables such as peas, corn, and potatoes, as well as dried beans, lentils, and peas, and grains like oats, barley, and rice. Grains are then further broken down into whole grains or refined grains. Eating whole grains ensures that you get all of the nutrients that whole grains offer. Refined grains are missing many vitamins and minerals.
Fiber
Fiber recommendations for people with diabetes are the same as for the general population. People should consume 14 grams of fiber per 1000 calories, or 25 grams for adult women and 38 grams for adult men, from a wide variety of sources daily. Of the recommended total fiber intake, 10 to 25 g/day should come from soluble fiber. Because of the potential beneficial effect of soluble fibers on blood lipids and glucose metabolism, people with diabetes are advised to get adequate amounts of fiber from the carbohydrates they eat. Fiber also contributes to digestive health, satiety, and the reduction of cholesterol levels. Good sources of soluble fiber include whole grains, fruits and vegetables, beans and legumes, rice bran and nuts.
Many research studies have attempted to identify optimal daily amounts of: carbohydrates, protein, and fat to manage diabetes; however there is not one optimal mix to manage diabetes. Instead, the best mix of carbohydrates, protein, and fat varies depending on the individual and must also take into consideration the weight management goals of the individual. There is not clear scientific evidence showing benefits of vitamin or mineral supplementation in people with diabetes without a nutrient deficiency, compared to the general population. Routine use of herbs and supplements is not recommended for people with diabetes due to lack of evidence. It is best to get the necessary vitamins and minerals from the foods you eat.
Alcohol
It is recommended that if adults with diabetes choose to consume alcohol, daily intake should be limited to a moderate amount (one drink per day or less for women and two drinks per day or less for men). Moderate alcohol consumption (when ingested alone) has little short term effect on glucose and insulin concentrations. However, carbohydrates consumed with alcohol, such as mixed drinks, can raise blood glucose. Individuals using insulin or medications that increase insulin secretion, who also consume alcohol, should consume food with the alcohol to reduce the risk of nocturnal hypoglycemia (low blood sugar levels at night). Check your blood glucose before you drink, while you drink, and for up to 24 hours to make sure you are at a safe level.
Physical Activity Recommendations
Regular physical activity is an important factor in diabetes management. It has been shown to improve blood glucose control, reduce cardiovascular risk factors, contribute to weight loss, and improve well-being. Exercise causes your cells to become more sensitive to insulin, and helps to remove glucose from the blood. People with diabetes should aim for 30 to 60 minutes of moderate to vigorous physical activity most days of the week. . This can be broken up throughout the week. In addition, individuals should perform aerobic exercise, muscle resistance training, stretching, and should become familiar with how their blood glucose responds to exercise. Before beginning a routine exercise program, people with diabetes should consult with their doctor.
Methods for Meal Planning
Glucose control is a balancing act. Carbohydrate foods raise blood glucose while insulin and physical activity lower blood glucose. To effectively control blood glucose, people with diabetes need to balance the amount of carbohydrate they eat, the type and amount of physical activity they do, and the diabetes medication they take. Dietary management of diabetes should be designed to meet total nutrient and health needs, not just blood glucose needs. The diet plan should begin with an assessment of the individual’s usual eating habits, including food likes and dislikes, eating and work schedules, as well as treatment goals identified by the health care team. The better dietary management fits into one’s usual routine, the more likely it is to be successful. The following diet planning systems can be helpful when planning meals and snacks for people with diabetes. The Plate Method is the recommended diet plan for people with diabetes. Other methods include diabetic exchange diets and carbohydrate counting.
Plate Method
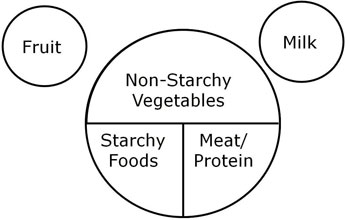 Figure 1: The Plate Method. |
The Plate Method is a simple method for tThe Plate Method is a simple method for teaching meal planning. A 9-inch dinner plate serves as a pie chart to show proportions of the plate that should be covered 1/2 –inch deep by various food groups. This meal planning approach is simple and versatile. Non-starchy vegetables (about 5 grams of carbohydrate) should cover 50 percent of the plate for lunch and dinner. One quarter of the plate should contain starchy vegetables and/or grains (1/2 cup or 1 oz. contains 15g of carbohydrate), including bread, grains, and potatoes. The final quarter of the plate should include a protein, including plant proteins, fish and seafood, poultry, cheese, and eggs. Finally, add a serving of fruit (1/2 cup is about 15g of carbohydrate) and some non-fat or low-fat milk (1 cup is about 12g of carbohydrate) are represented outside the plate. Overall, choose healthy fats like nuts, seeds, and avocados, and cook with oils. To complete your meal, add a low-calorie drink like water, or unsweetened tea.
Diabetic Exchange Diets
In this system, food is separated into six categories based on macronutrient content (i.e., starch [cereals, grains, pasta, bread, beans, and starchy vegetables], meat and meat-substitutes, non-starchy vegetables, fruits, milk and fats). Individuals, with the help of a physician or dietitian, design a daily meal plan based on a set amount of servings from each category. The exchange method allows a person to measure rather than weigh food. This saves time and encourages compliance. Any food may be substituted for another within the same food exchange list. As with other methods, all meals and snacks should be eaten at about the same time each day and be consistent in the amount of food consumed.
Figure 2: Diabetic Exchange List
| Carbohydrate (grams) |
Protein (grams) |
Fat (grams) |
Calories | |
| I. Starch/Bread | 15 | 3 | trace | 80 |
| II. Meat | ||||
| Very Lean | – | 7 | 0-1 | 35 |
| Lean | – | 7 | 3 | 55 |
| Medium Fat | – | 7 | 5 | 75 |
| High-Fat | – | 7 | 8 | 100 |
| III. Vegetable | 5 | 2 | – | 25 |
| IV. Fruit | 15 | – | – | 60 |
| V. Milk | ||||
| Skim | 12 | 8 | 0-3 | 90 |
| low-fat | 12 | 8 | 5 | 120 |
| Whole | 12 | 8 | 8 | 150 |
| VI. Fat | – | – | 5 | 45 |
Carbohydrate Counting
Some people choose to count the grams of carbohydrate in various foods and adjust the amount of carbohydrate consumed during the day as a reflection of blood glucose levels. One serving from the starch, fruits, milk, or sweets and dessert list supplies about 15 grams of carbohydrate. Each selection is considered one carbohydrate choice. A meal plan outlines the number of carbohydrate choices a person may select for meals and snacks. With carbohydrate counting, always include a source of protein and healthy fat for a balanced meal. This method requires great diligence with diet and blood glucose monitoring.
Dietary Guidelines/MyPlate
MyPlate strives to put the 2015-2020 Dietary Guidelines for Americans into action. It provides a conceptual framework for selecting the kinds and amounts of various foods, which together provide a nutritious diet. MyPlate focuses on variety, amount, and nutrition. Balance calories by enjoying foods but eating less and avoiding oversized portions. Foods to increase are fruits, vegetables, whole grains, and non-fat or low-fat dairy. Foods to reduce are saturated fat, sodium, and added sugars.
Using Nutrition Labels
With any of the diet planning methods mentioned above, the nutrition facts label found on most foods can provide useful information. If counting carbohydrates, total grams of carbohydrates per serving are listed on the label, along with grams of sugars and dietary fiber. Be aware that the serving sizes given on labels may not be the same as those used in the Exchange Lists for Meal Planning. For example, the label serving size for orange juice is 8 fluid ounces (1 cup). In the Exchange Lists, the serving size is 4 ounces (1/2 cup). Thus, a person who drinks 1 cup of orange juice has consumed two fruit exchanges. If using MyPlate in menu planning, pay close attention to the percent daily value column of the nutrition facts label. Look for foods that have low percent daily values for saturated fat, and low amounts of sugar, and high percent daily values for fiber. And choose items with no trans fats.
| For More Information:
American Diabetes Association: |
Diabetes is a complex disease. With the proper treatment considering a healthful eating pattern, physical activity, and pharmacological therapy, the disease can be effectively managed. Maintaining near normal blood glucose, blood lipid, and blood pressure levels can prevent short term and long term complications associated with diabetes. There are many treatment plans to manage diabetes, which may be tailored to best meet the individual’s needs.
References
Position Statement of the American Diabetes Association. Nutrition Therapy Recommendations for the Management of Adults with Diabetes. Diabetes Care. 2013; Volume 36.
Position Statement of the American Diabetes Association. Standards of Medical Care in Diabetes – 2012. Diabetes Care. 2012; Volume 35, Supplement 1.
National Center for Chronic Disease Prevention and Health Promotion. National Diabetes Fact Sheet, 2011. Centers for Disease Control and Prevention. 2011.
Lorenzo, C., Williams, K., Hunt, K.J., Haffner, S.M. The National Cholesterol Education Program–Adult Treatment Panel III, International Diabetes Federation, and World Health Organization Definitions of the Metabolic Syndrome as Predictors of Incident Cardiovascular Disease and Diabetes. Diabetes Care. 2007; Volume 30, Supplement 1.
Stone, N.J., Bilek, S., Rosenbaum, S. Recent National Cholesterol Education Program Adult Treatment Panel III Update: Adjustments and Options. The American Journal of Cardiology. 2005; Volume 96, Issue 4.
Stone, N.J., Bilek, S., Rosenbaum, S. Recent National Cholesterol Education Program Adult Treatment Panel III Update: Adjustments and Options. The American Journal of Cardiology. 2005; Volume 96, Issue 4.
*Original fact sheet by L. Bellows, Colorado State University Extension foods and nutrition specialist and assistant professor, food science and human nutrition; K. Nichols, graduate intern, food science and human nutrition. 8/03. Revised 8/17.
Colorado State University, U.S. Department of Agriculture, and Colorado counties cooperating. CSU Extension programs are available to all without discrimination. No endorsement of products mentioned is intended nor is criticism implied of products not mentioned.
Go to top of this page.





